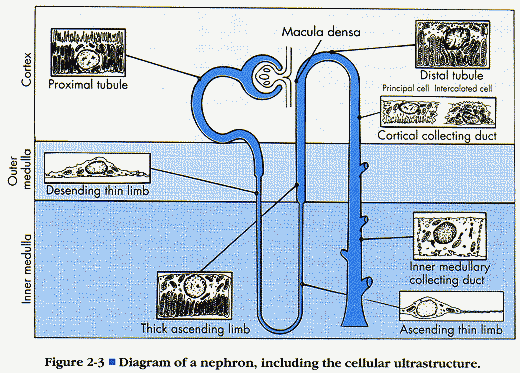
Koeppen and Stanton. Renal Physiology, 2nd Edition, Mosby: St Louis, p. 21 (Figure 2-3).
(Ch. 1 and 2, Koeppen and Stanton)
Have a good understanding of the basic anatomy of the two major types of
nephrons (juxtamedullary and cortical), particularly the different segments that
constitute each type of nephron. The nephron is the functional unit of
the kidney, with each kidney containing 1.0 to 1.3 million nephrons. Each
consists of a glomerular capillary network (glomerulus) that is surrounded by a
Bowmans’s Capsule. Both of these together equal a renal corpuscle. The
nephrons are named from where the nephron originates – Cortical or
Juxatmedullary.
Each nephron consists of:

Koeppen and Stanton. Renal Physiology, 2nd Edition, Mosby: St
Louis, p. 21 (Figure 2-3).
Have an understanding of the blood supply to the kidney, including the vasa recta and peritubular capillary networks, and their importance. Blood enters the kidney via the renal artery which branches a number of times into segmental arteries which subdivide into interlobar arteries. Each interlobar artery penetrates the kidney through a "column of Berlin". Before reaching the cortical surface it divides into arc-shaped arcuate arteries which run parallel to the surface. Interlbular arteries (or cortical radial arteries) arise from the arcuate arteries and penetrate the cortex perpendicularly toward the surface. Branching from each interlobular artery are the afferent arterioles, which enter Bowman’s Capsule.
Juxamedullary nephrons have glomerulli which arise in the deep cortical regions. Their loops of Henle extend deeper into the kidney, going into the inner medulla varying distances. The efferent arteriole of the juxamedullary nephron continues as a peritubular capillary bed, but also gives rise to a series of vascular loops called the vasa recta. These descend to varying depths to the inner medulla and break up into capillary networks, especially around the ascending thin limb of the loop of Henle.
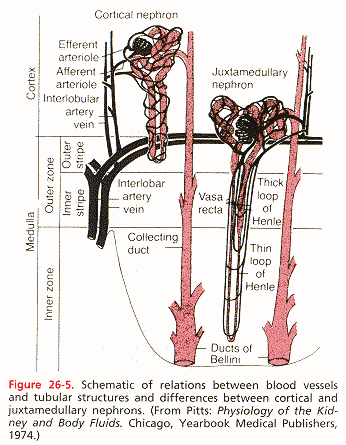
Guyton and Hall. Textbook of Medical Physiology, 9th Edition.
WB Saunders Company: Philadelphia, p. 318
Be clear in your mind on the difference between the terms "reabsorbtion", "secretion", and "filtration", which describe the handling of water and solute in the nephron, and the direction in which it they are transported.
Have an idea of what the juxtaglomerular apparatus (JGA) is, and what it’s role in renal function is in the so-called "renin-angiotensin-aldosterone" cascade.
The juxtaglomerular apparatus (JGA) is the part of the nephron where
the distal tubule of a nephron loops back up and passes between its vascular
pole (where the afferent arteriole enters and the efferent arteriole leaves the
glomerulus). Specialized epithelial cells (macula densa cells) line the lumen of
the early distal tubule. The macula densa cells contact the extraglomerular
mesangial cells and granular cells of the afferent and efferent arterioles. The
granular cells are modified smooth muscle cells that manufacture, store, and
release renin. Changes in sodium composition and probably flow rate of the
filtrate are sensed by the macula densa cells which send the signal to the
granular cells to ![]() or
or ![]() renin secretion. Renin is usually secreted in response to a ¯
in plasma volume which will activate the renin-angiotensin-aldosterone cascade.
renin secretion. Renin is usually secreted in response to a ¯
in plasma volume which will activate the renin-angiotensin-aldosterone cascade.
Know what the major body fluid compartments are (total body water [TBW], extracellular fluid [ECF], and intracellular fluid [ICF]), and how they relate to each other. Know how to calculate a rough estimate of their size if you were given a body weight in kilograms.
Sixty (60%) of total body weight is composed of water (approximately 42
liters in the average 70 kg adult male).
Total body water is distributes primarily between two compartments:
About 28 liters (67%) of the 42 liters are contained within the cells (ICF). The remaining 14 liters (33%) is comprised of the ECF.
The ECF is divided into 2 major subdivisions:
Also classified as ECF: crystallized water in bone and fluid in dense connective tissues (Other minor ECF compartments: GI, biliary, urinary tracts, intraocular, CSF, pleural, peritoneal, cartilage), pericardial fluids.
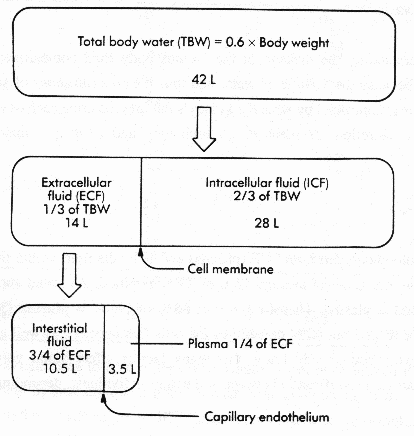
From Class Handout
Estimating volumes:
TBW (L) = 0.6 x body wt (kg)
ICF (L) = 0.4 x body wt (kg)
ECF (L) = 0.2 x body wt (kg)
|
Express ICF and ECF as % of TBW: |
If know ICF and/or ECF can estimate TBW: |
|
ICF = .67 x TBW (in L) |
TBW = ICF (L) / .67 |
|
ECF = .33 x TBW (in L) |
TBW = ECF (L) / .33 |
Understand what osmolality and osmolarity are, and why water and solute
shift between the ECF and ICF the way they do when either hypotonic, hypertonic,
or isotonic fluids are added to the ECF, as shown in a figure 25.6 near the end
of the first handout ("Overview of the Major Components of Renal
Function").
Osmolality: the number of solute particles in 1 kg of water.
Osmolarity: the number of solute particles per 1 liter of water.
For dilute solutions, the difference between them is insignificant.
Measurements of osmolarity are temperature dependent, because the
volume of water varies with temperature (volume is higher at higher
temperature).
Osmolality is based on the mass of water so it is temperature
independent.
Osmolality has units of osm/kg H2O. Because of the dilute nature of
physiologic solutions – osmolalities are expressed as milliosmoles per
kilogram water (mOsm/kg H2O).
Summary:
Isotonic – change in volume only of ECF.
Hypotonic – change in increase of volume of each compartment, osmolality of
each ![]() .
.
Hypertonic – total volume of ICF ![]() ; total volume of ECF
; total volume of ECF ![]() ; osmolality of both
; osmolality of both ![]() .
.
Last Updated 09/06/01 08:53:30 PM
Return To The MNA 2001 Homepage